The Pre-Care Estimate API enables dental providers to receive real-time cost estimates from dental payers prior to treatment, helping reduce denials and improving patient cost transparency. By integrating directly into existing workflows, this centralized API provides access to critical pre-treatment information such as eligibility, prior authorization requirements, and payer-specific policies, so providers can deliver accurate estimates and give patients a clearer picture of what they will owe before care.
For UnitedHealthcare, this process runs as a trial claim, while for all other payers, it functions as a pre-treatment estimate. This helps improve patient experience, reduce surprises, and streamline reimbursement. The end-to-end validation helps reduce claim rejections, improve first-pass yield, and accelerate reimbursement.
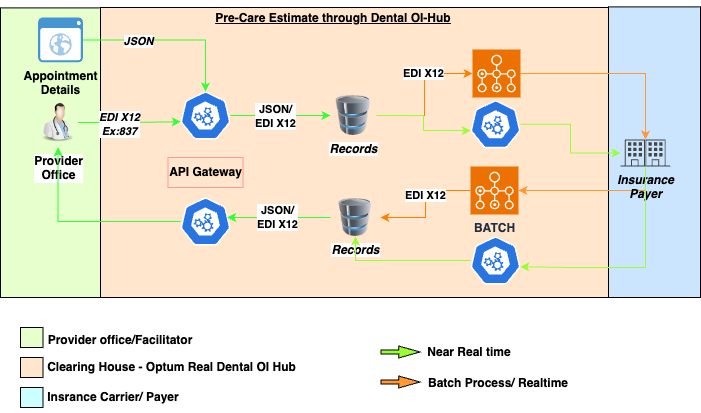
Real Pre-Care Estimate Flowchart
Key features
- Validates that a specific member record exists
- Checks eligibility for membership coverage for the date of service
- Pre adjudication check for:
- Prior Authorization requirements and status
- Member Benefits details
- Compliance with payer-specific payment and dental policies
- HIPAA-compliant X12 formatting